Risks of Rubbing Your Eyes While Wearing Contact Lenses
The Unconscious Habit That Puts Your Vision at Risk
It’s a reflex we seldom think about. An itch, a feeling of dryness, or a stray eyelash triggers an immediate, almost unconscious response: we rub our eyes. For most people, it’s a harmless habit. But for the 45 million Americans who wear contact lenses, this simple act can introduce serious, sight-threatening risks. Rubbing your eyes with contacts in is one of the most common yet dangerous mistakes a wearer can make.
This article provides a definitive guide to understanding the mechanical and microbial dangers of eye rubbing. We will explain exactly what happens to your eye and the lens when you apply pressure, explore the root causes of the irritation that leads to rubbing, and provide a safe, step-by-step protocol for relief. Mastering this simple skill is not just about comfort—it's a fundamental practice for ensuring the long-term health of your eyes.
TL;DR: The Safe Way to Handle an Itchy Eye with Contacts
- Never Rub: Rubbing can fold or dislodge your lens, turning its delicate edge into a tool that can scratch your cornea. It also transfers germs from your fingers directly onto the lens.
- The Real Cause: The urge to rub is almost always caused by dryness, which makes the lens adhere less smoothly to the eye. Allergens or protein deposits are other common culprits.
- Safe Relief Protocol: When you feel an itch, stop. Forcefully blink several times, then apply preservative-free lubricating drops formulated for contact lenses. This rehydrates the lens and flushes out irritants.
- Repositioning a Lens: If a lens feels out of place, add more lubricating drops, close your eye, and gently massage your eyelid—not the eyeball itself—to guide the lens back into position.
The Mechanical Dangers: What Happens When You Rub?
When you wear a contact lens, you place a precisely engineered medical device on the surface of your cornea, one of the most sensitive tissues in your body. Applying external pressure through rubbing disrupts this delicate interface, creating several immediate physical risks.
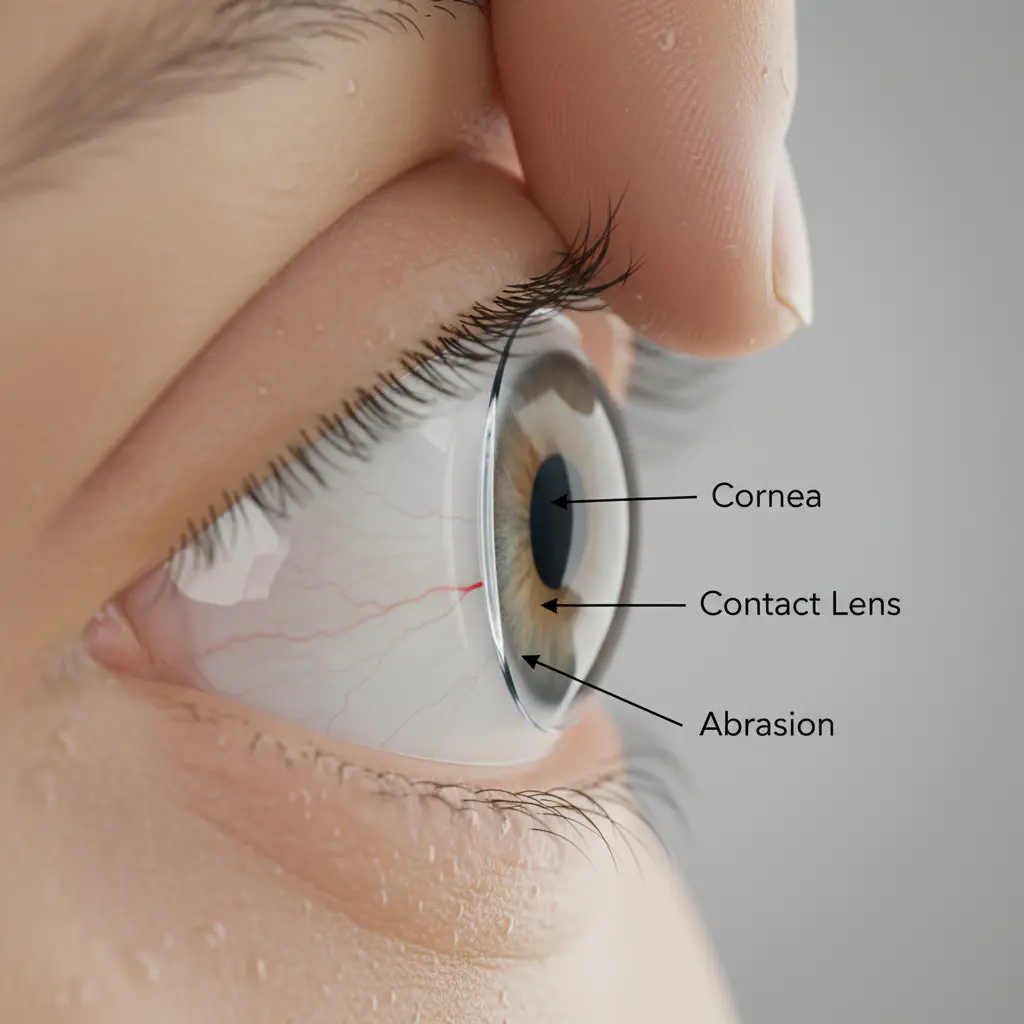
1. Corneal Abrasion: The Sandpaper Effect
The surface of your eye, the cornea, is a smooth, transparent dome. A properly hydrated contact lens floats on a thin layer of tears, moving harmlessly with each blink. However, when the eye or lens becomes dry, this cushion vanishes.
Rubbing a dry lens against a dry cornea is like rubbing fine-grit sandpaper on a delicate surface. According to the National Eye Institute (NEI), the cornea is essential for focusing vision and is comprised of highly organized cells and proteins. A scratch on this surface, known as a corneal abrasion, can cause significant pain, redness, light sensitivity, and blurry vision. While most minor abrasions heal, they create a temporary breach in the eye's primary defense, leaving it vulnerable to infection.
2. Lens Displacement, Folding, and Tearing
The friction from rubbing can easily overcome the forces holding a soft contact lens in place. The lens can fold in half, get trapped under the upper or lower eyelid, or even be expelled from the eye completely. A folded lens causes immediate blurry vision and discomfort. While a "lost" lens is almost always tucked away under an eyelid, the experience can be alarming. More aggressive rubbing can cause a small tear in the lens itself, creating a sharp edge that can further damage the eye.
3. Introducing Harmful Microbes
Your hands carry a significant load of bacteria, fungi, and other germs. The Centers for Disease Control and Prevention (CDC) explicitly warns that these microbes can cause serious eye infections. A landmark study published in the Morbidity and Mortality Weekly Report found that a staggering 99% of contact lens wearers report at least one hygiene risk behavior.
When you rub your eyes, you are manually pressing this contamination from your fingers and eyelashes directly onto the lens surface. From there, it's a short journey to the cornea. If a microscopic abrasion is already present, these germs have a perfect entry point to cause microbial keratitis—a severe infection of the cornea that can lead to corneal ulcers and, in rare cases, permanent vision loss.
The Root Cause: Understanding Why Your Eyes Itch
The urge to rub is a symptom, not the core problem. Addressing the underlying cause of the irritation is the most effective way to break the habit. For contact lens wearers, the culprits are usually environmental and physiological.
- Contact Lens Induced Dry Eye (CLIDE): This is the most common cause. Contact lenses can disrupt the natural tear film that keeps your eyes moist and comfortable. Long hours in air-conditioned or heated spaces, coupled with reduced blink rates during screen time, accelerate this drying effect. A dry lens feels like a foreign object, triggering the itch response.
- Trapped Allergens and Debris: Microscopic particles like pollen, dust, and pet dander can get caught between the lens and the cornea. The lens acts like a tiny dome, preventing your natural tears from flushing the irritant away, leading to persistent itching and inflammation.
- Protein and Lipid Deposits: Your tears naturally contain proteins and lipids that can build up on the surface of your lenses over the course of the day or month. These deposits create a rough, irritating surface. This is why the "rub and rinse" step when cleaning reusable lenses is non-negotiable for removing these stubborn buildups.
The Safe Response Protocol: A Step-by-Step Guide to Relief
Your first instinct is often your worst enemy. Instead of rubbing, commit the following three-step protocol to memory. This is the method eye care professionals recommend for safely managing irritation without causing harm.

Step 1: The "Blink and Wait" Rule
The moment you feel an itch or the sensation of something in your eye, stop what you are doing. Do not touch your eye. Instead, blink hard and deliberately five or six times. This action does two things: it stimulates your natural tear glands to produce more moisture, and the motion of the eyelid can help reposition a slightly displaced lens or dislodge a tiny particle. Wait about 30 seconds to see if the sensation subsides.
Step 2: Lubricate with Rewetting Drops
If blinking alone doesn't resolve the issue, the next step is to introduce moisture. Always use a sterile, preservative-free rewetting solution specifically labeled as safe for contact lenses.
- Wash your hands thoroughly.
- Tilt your head back and gently pull down your lower eyelid.
- Instill one or two drops directly into the eye, avoiding touching the bottle tip to your eye or eyelid.
- Close your eye for a few moments to allow the solution to spread evenly over the lens surface.
This instantly rehydrates the lens, restores the tear cushion, and helps flush out any trapped debris. For many, this provides immediate and complete relief.
Step 3: The Closed-Eyelid Massage for a Displaced Lens
If the lens still feels out of place (e.g., you feel a bump under your upper eyelid), do not try to force it out.
- Add another one or two lubricating drops to the eye. This is critical to ensure the lens can move freely.
- Close your eye.
- Look in the direction opposite to where you feel the lens. If you feel it at the top of your eye, look down towards your cheek.
- Using your fingertip, apply very gentle pressure to your closed eyelid and massage in a slow, circular motion. This uses the smooth, lubricated inner surface of your eyelid to gently guide the lens back toward the center of your cornea.
When to Remove Your Lenses—and When to Wait
Knowing when to take a lens out is just as important as knowing how to manage irritation. Rushing to remove a lens from a painful eye can sometimes make things worse.
Follow the 5-Minute Rule: If you have tried the lubrication protocol and your eye is still red, painful, or your vision remains blurry after five minutes, it is time to remove the lens.
However, it is crucial to lubricate the eye before removal. If you have inadvertently caused a small scratch, pulling a dry lens across the cornea can aggravate the abrasion. Adding a drop of solution first ensures the lens will slide off with minimal friction.
After removing the lens, examine it for tears or debris. Clean and disinfect it thoroughly if it is a reusable lens. If your eye remains irritated after removal, give it a rest and wear your glasses. If symptoms worsen or do not improve, contact your eye doctor immediately.
Seek immediate medical attention if you experience:
- Severe, throbbing eye pain
- Extreme sensitivity to light
- Thick, colored discharge from the eye
- A sudden, dramatic decrease in vision
These can be signs of a corneal ulcer or serious infection, which the U.S. Food & Drug Administration (FDA) warns requires urgent treatment to prevent permanent vision damage.
Frequently Asked Questions
-
What if my contact lens is really stuck under my eyelid? Stay calm. A soft lens cannot get lost behind your eye. Follow the lubrication and closed-eyelid massage protocol. Adding plenty of rewetting drops is the key to getting it to move. If you cannot retrieve it, see your eye doctor.
-
Can rubbing my eyes with contacts really cause a serious infection? Yes. The link between poor hygiene and infection is well-established. The CDC notes that serious eye infections can lead to blindness and affect up to one in every 500 contact lens wearers per year. Transferring germs via rubbing is a primary risk factor for developing microbial keratitis.
-
My eyes are always dry and itchy by the end of the day. What can I do? This is a very common issue. First, ensure you are using rewetting drops throughout the day. Second, talk to your eye doctor. They may recommend switching to a lens material with higher oxygen permeability, like silicone hydrogel, or moving to a daily disposable lens. As we discuss in our article, daily disposable lenses can often help with dry eyes by providing a fresh, clean, and highly hydrated lens every single day.
-
What kind of eye drops are safe for my contacts? Only use products specifically marked as "for contact lenses" or "rewetting drops." Never use anti-redness drops (vasoconstrictors) or allergy drops while wearing your lenses unless approved by your doctor, as their preservatives can bind to the lens material and cause irritation. Preservative-free formulas are the gentlest and safest option for frequent use.
Breaking the reflexive habit of rubbing your eyes is one of the most important skills you can develop as a contact lens wearer. By understanding the risks and adopting a safe protocol of blinking, lubricating, and gentle massage, you protect your cornea from damage and infection. Treat your contact lenses as the medical devices they are, and prioritize clean hands and proper hydration to ensure your eyes remain comfortable and healthy for years to come.
Disclaimer: This article is for informational purposes only and does not constitute professional medical advice. Always consult with a qualified eye care professional for any health concerns, before starting any new treatment, or with questions about your specific medical condition. Do not disregard professional medical advice or delay in seeking it because of something you have read in this article.
References
- Centers for Disease Control and Prevention (CDC). "Healthy Contact Lens Wear and Care." Retrieved from https://www.cdc.gov/contact-lenses/index.html
- U.S. Food & Drug Administration (FDA). "Contact Lens Risks." Retrieved from https://www.fda.gov/medical-devices/contact-lenses/contact-lens-risks
- Cope, J. R., Collier, S. A., et al. (2017). "Contact Lens Wearer Demographics and Risk Behaviors for Contact Lens-Related Eye Infections — United States, 2014." Morbidity and Mortality Weekly Report, 66(32), 841–845. Retrieved from https://www.cdc.gov/mmwr/volumes/66/wr/mm6632a2.htm
- National Eye Institute (NEI). "Parts of the Eye." Retrieved from https://www.nei.nih.gov/learn-about-eye-health/healthy-vision/parts-eye




















